AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
Back to Blog
Cervical spine x ray icd 104/5/2024 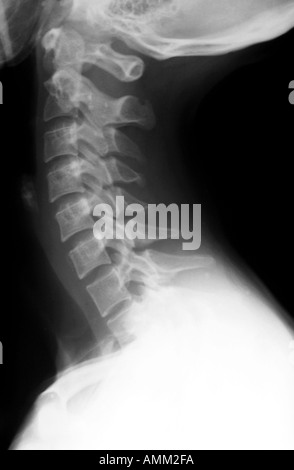
Associated disruption of the C2 to C3 disc with a Hangman fracture requires surgical fixation. Fracture through the C2 dens can be classified as type I, II, or III. If the fracture is displaced greater than 3mm or with greater than 11 degrees of angulation, reduction with halo placement or surgical fixation should be considered. Hangman fracture with less than 3mm of displacement and no significant angulation may be treated in a hard cervical collar. If the fracture extends bilaterally through the pars interarticularis, a Hangman fracture is described. Ĭ2 fractures can result in a fracture through the body, dens, or pars. If the TAL is disrupted C1 to C2 posterior fusion should be considered. C1 fractures may be managed in a rigid cervical collar or halo if the transverse alar ligament (TAL) remains intact on MRI. Neurological injury rarely results from an isolated C1 fracture due to abundant space surrounding the spinal cord. Fractures of C1 occur through the lateral mass or arch in single or multiple places (multiple arch fractures, Jefferson fracture). Injuries to C1 and C2 compose approximately 30% of cervical spine fractures. 
A SLICS score of 1 to 3 is nonsurgical, a score of 4 is not specified, and a score of 5 or greater is a surgical indication. Scoring systems in dealing with cervical spinal cord injury that includes ligamentous, bony and neurologic injury exist, a common one is called SLICS (Subaxial Cervical Spine Injury Classification System), and this can be used to help with evaluation and guidance of surgical or nonsurgical management. Further evaluation of ligamentous structures of the spinal cord with MRI is important for determining spinal stability and in planning surgical treatment. Computed tomography is the preferred imaging in acute spine trauma as it is more sensitive for detection of bony cervical spine injury when compared to plain radiographs (sensitivity of 98% versus 52%). However, in neurologically stable patients, if there is significant disc prolapse, discectomy, or corpectomy is carried out (to prevent cord injury when the patient is in the prone position), then the posterior approach to unlock the facets and posterior instrumentation is the appropriate procedure, followed again by the anterior approach to bony graft placement along with plate and screw fixation (360-degrees approach) is warranted.Indications for cervical spine imaging include localized neck pain, deformity, edema, altered mental status, head injury, or neurological deficit. This approach can be reinforced with fixation from the anterior approach as well. However, in patients with ASIA 'C' and 'D' status, the posterior approach is necessary to first to unlocking the jammed facet, and the anatomical fixation is carried out following lateral mass and translaminar screw and rod fixation. If reduction fails in patients with ASIA 'A' and 'B' status, posterior-only fixation by interspinous wiring is justified for anatomical fixation to aid in early rehabilitation. Sometimes, owing to financial barriers, simple graft placement can also be undertaken. In cases of failed reduction from traction, the clinician can attempt reduction following muscle relaxation after induction of anesthesia. If there is a good reduction following traction, the patients can receive an anterior approach with discectomy or median corpectomy followed by in-situ bony graft fusion or the usage of allograft spacers aided with plate and screw fixations. 
The treatment algorithm is also determined by the patient's characteristics as well as the expertise of the team. The anterior approach is better suited to deal with the herniated disc, whereas the posterior approach helps restore the posterior tension band. The surgical plan in the management of the patient then varies according to the Meyerding grading system, the ASIA neurological status, and the relevant scoring system of the patient. The failure of reduction needs the posterior reduction of the jumped facets, followed by 360-degree global fixations in neurologically preserved patients. The reduction can then take place by anterior-only fusion. If there is no reduction and the preoperative MR images show the presence of disc prolapse, an anterior approach is the next step, with discectomy followed by open reduction with the aid of a Casper distractor. In cases with locked facets, the clinician should attempt a closed reduction under anesthesia, which is successful in almost 95% of cases. Reduction of the grade of the subluxation in cases of reducible locked facet jointsĬare always needs to avoid cord traction due to heavy tractional weights.
0 Comments
Read More
Leave a Reply. |
 RSS Feed
RSS Feed
